 
Patients with increased floaters and/or flashes should be evaluated by a retinal specialist at the earliest to check for the development of PVD, retinal tears, or retinal detachment. With this background, this article aims to provide a set of guidelines for the management of retinal degenerations in eyes undergoing refractive surgeries.įollow-up retinal examination schedule after refractive surgeryįollowing microtome-assisted LASIK or femtosecond-assisted LASIK, a PVD can occur as early two days post-surgery in 16% of cases and in up to 85% within a month. While there are guidelines for the treatment of symptomatic and asymptomatic retinal breaks and lattice degeneration, there are no clear guidelines for retinal screening and management of asymptomatic retinal degenerations prior to refractive surgery or for follow-up of these patients.  
Given the high incidence of refractive errors (123.7 million) worldwide, and with over 13 million LASIK procedures having been performed in the United States alone, the numbers seeking refractive surgery are only going to increase. Prophylactic treatment of retinal degenerations which can predispose to retinal tears is advisable. A retinal examination of myopic eyes, both pre- and post-operative, is therefore mandatory. Irrespective of the refractive error grade or the procedure done, a PVD can lead to retinal tears and an RRD. Thus, one can assume that the incidence of PVD following SMILE is less compared to LASIK or femtosecond LASIK. In the SMILE technique, there are no fluctuations in the intraocular pressure as in LASIK. It is reported to achieve similar optical effects femtosecond LASIK with excellent postoperative outcomes. In this flap-less procedure, a corneal lenticule is created using a femtosecond laser and then extracted through a small incision. Small incision lenticule extraction is a relatively new refractive procedure designed to treat a range of refractive errors. This may be due to a longer suction time during femtosecond LASIK despite a lower suction pressure. Even in newer surgical techniques like the femtosecond LASIK, the incidence of PVD occurrence or progression is either higher or comparable to that seen in the microkeratome LASIK cohort of patients. Many patients complain of increased floaters (PVD) after LASIK. These have the potential to cause changes in the vitreous, retina, and macula. During laser-assisted refractive surgeries like LASIK, there are significant ocular mechanical stressors like an increase in intraocular pressure (>65 mm Hg) during application of the microkeratome suction ring, an acoustic shock wave during the laser ablation, and a rapid lowering of intraocular pressure when the suction ring is decompressed. A posterior vitreous detachment (PVD) is also more common in myopes and present at a much younger age. 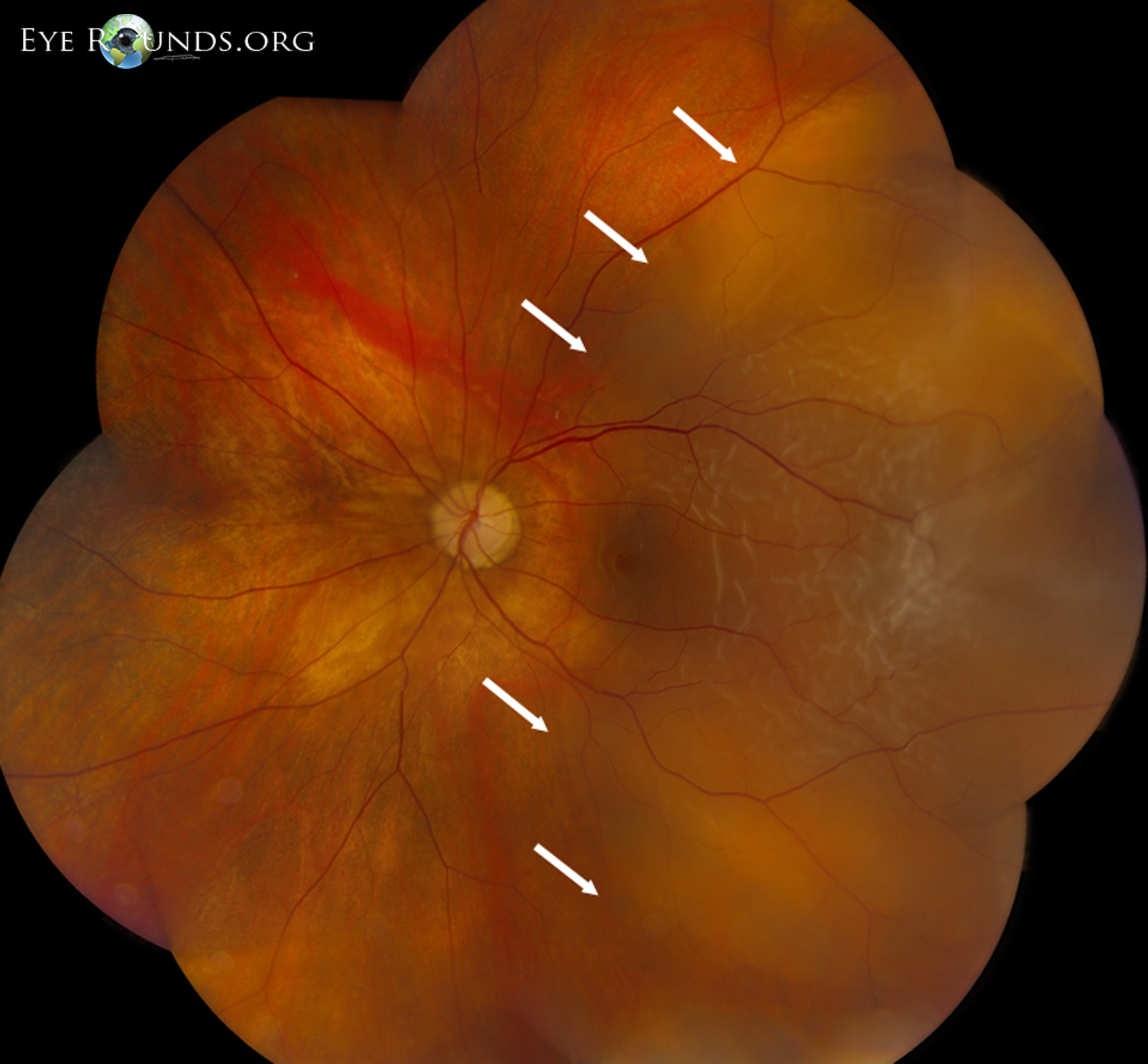
Lattice degeneration, snail-track degeneration, retinal tears/holes, degenerative retinoschisis, cystic retinal tufts, and, rarely, zonular traction tufts, can result in a rhegmatogenous retinal detachment (RRD) and its associated morbidity. Newer procedures like small incision lenticule extraction (SMILE) are gaining popularity for the correction of myopia.ĭegenerations involving the peripheral retina are common in myopes and studies have shown a higher prevalence with increasing grades of myopia. Other less commonly used refractive surgeries include radial keratotomy, thermal conductive keratoplasty, automated lamellar keratoplasty, and epikeratoplasty. The different refractive surgical techniques used in the treatment of myopia include surface ablation techniques like photorefractive keratotomy, laser in-situ keratomileusis (LASIK), femtosecond LASIK and intraocular procedures like intrastromal corneal ring segments, phakic intraocular lens (phakic IOL) and elective refractive lens exchange. Since the past several decades, surgical correction of refractive errors, particularly myopia, is on the rise. There is either a steep cornea or a longer axial length or a combination of both in myopia. Refractive errors seen in day-to-day clinical practice include myopia, hyperopia, astigmatism, and presbyopia of which, myopia is the most common. Uncorrected refractive errors continue to be the most common cause of moderate to severe visual impairment in young adults. 
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
